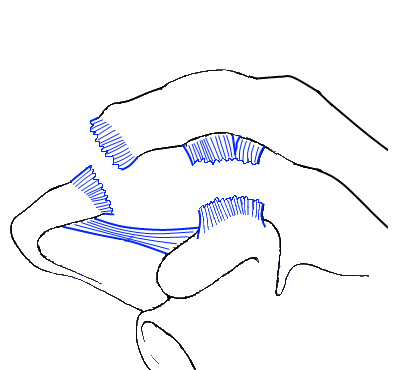
Careful dissection is made subcutaneously to the pronator teres fascia (Fig. A 2–3-cm transverse incision is placed in the flexion crease of the cubital fossa, from 1 cm medial of the biceps tendon to 2 cm lateral of the medial epicondyle (see Fig. 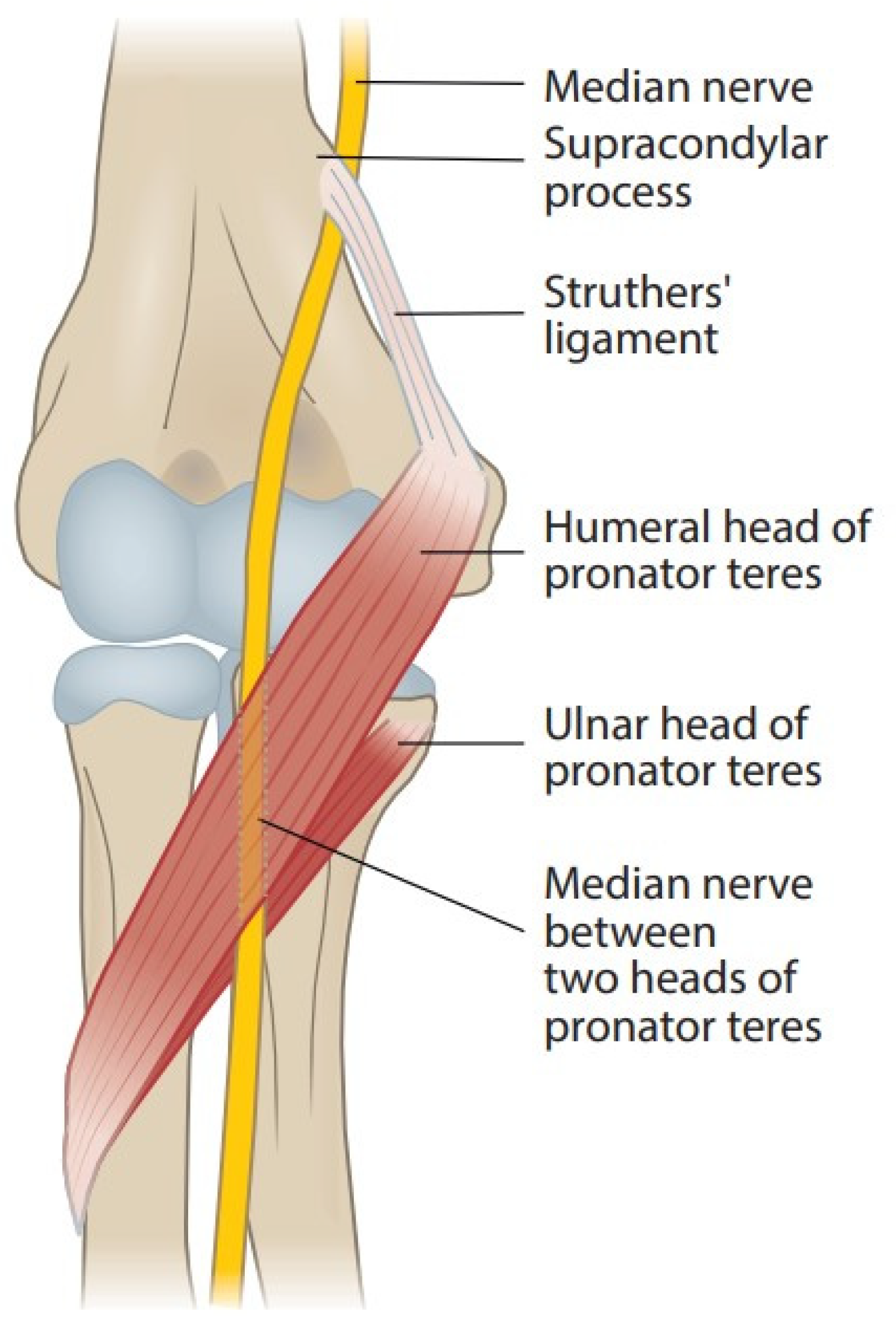
The surgery is performed with the patient awake and no tourniquet. In the case of PMNE, these patterns have been determined to primarily correlate to weakness in the flexor pollicis longus (FPL), flexor digitorum profundus II (FDP II), and the flexor carpi radialis (FCR). The principle is easy: distal to the level of nerve affliction, distinct patterns of muscle weaknesses will be clinically present. The efficacy (sensitivity and specificity) of manual muscle testing of antagonist muscles to determine levels of focal neuropathies in the upper extremities have been established in randomized, blinded validity studies to 88–93 %, respectively. 
Similarly, the earliest publications on PMNE describe the need of thorough physical examination to diagnose the patient, in particular the presence of weakness in muscles innervated by the median nerve both in the hand and the forearm. The objective of this manuscript is to revisit the clinical findings and diagnosis of PMNE, as well as describe an in situ approach to surgical decompression of the median nerve at the elbow, with video guidance.Īlready in 1874, Erb emphasized the importance of clinical diagnosis for determination of level of nerve affliction in the upper extremity. More recently, magnetic resonance imaging (MRI) has been suggested as a potential aid in proximal entrapment diagnosis, but in the case of PMNE, the MRI findings are usually normal until there is evident axonal degeneration and muscle wasting of the forearm. The shortcomings of electrodiagnostic studies lies in the fact that a nerve may be compressed and cause symptoms distal to the level of compression due to changes in axonal transport and intraneural circulation, but the pressure levels of compression are too low to actually cause axonal injury and thus no visible changes in EMG/NCS. In the case of PMNE, however, there is a conundrum in that proximal median EMG/NCS often is normal or inconclusive, may simulate CTS, and has an unreliable specificity of 30–70 %. In what lies the elusiveness of this diagnosis? In this age of insurance-driven medicine, the dependency on so-called objective measurements, i.e., electromyography (EMG) and nerve conduction studies (NCS), is brought to the forefront of medicine whereas clinical diagnosis and examination is often considered subjective, biased, and unreliable. This disparity has led surgeons to claim that PMNE is an “extremely rare diagnosis” and a “diagnosis of belief or disbelief”, as objective measurements of PMNE can seldom be retrieved. The pronator syndrome, or proximal median nerve entrapment (PMNE) at the level of the elbow, was first described in literature in the 1950s, but unlike its distal counterpart-the carpal tunnel syndrome (CTS)-there are only around 50 publications on the diagnosis and treatment of PMNE, whereas a PubMed search on CTS will result in >7,500 publications.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
